25/9 By Jaydev Varma, Head of Product
People-centric diabetes virtual care
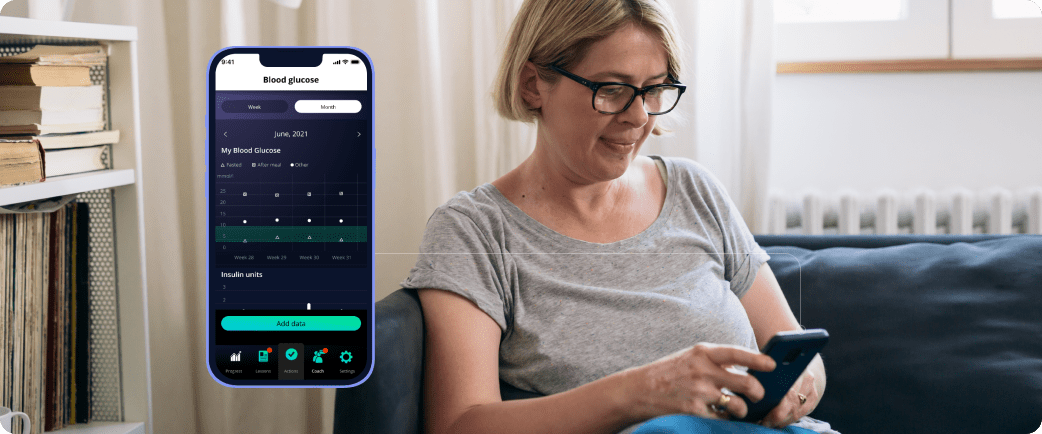
In the Netherlands, we are still in the early stages of using technology in outpatient chronic care to improve outcomes at scale. In the case of type 2 diabetes, wider adoption cannot come soon enough, given the growing numbers of people with the disease – and the related socioeconomic impact.
Diabetes: A mounting public health challenge
Over 1.1 million Dutch citizens suffer from type 2 diabetes (T2D), and this number is growing by about 1200 a week, partly driven by a rise in the number of people – of all age groups – who are overweight or obese. The annual spend on diabetes is around €6.8 billion, a quarter of which pertains to direct healthcare costs. Fueled by the growth in patient volumes as well as inflation, these costs are estimated to treble in the years ahead.
Diabetes care in the Netherlands (and many other countries) is mostly a reactive process – punctuated by planned or unplanned patient visits. It is also labor-intensive. People with diabetes represent around 5% of the total number patients, yet they account for 12-15% of a typical GP’s workload – a disproportionate impact on a system already stressed by unfilled vacancies and rising costs.
T2D also takes its toll on the quality of life and productivity of individual patients, as well as on their families, who often play the role of (informal) caregivers. The progressive nature of the disease, together with comorbidities, may also result in worsened health and earlier death, burdening the patients and their loved ones with further hardships.
Though a sobering reminder, this message has been repeated often enough that few healthcare professionals and policymakers would deny the scale of the T2D problem and its implications. Despite this knowledge and urgency, diabetes care appears to be falling short, as reflected by the growing numbers and costs. Without addressing the underlying factors that contribute to the disease and ensuing complexities, reliance on pharmaceuticals to reduce symptoms will not have a positive impact, either economically or in terms of patients’ wellbeing.
Lifestyle medicine: More than a silver lining

While T2D cannot be cured completely, with timely lifestyle changes and consistent self-management to maintain blood glucose levels within a healthy range, over 40% of patients can lead normal lives, avoiding the need for insulin or medication, non-elective healthcare visits, or loss of productivity. And even if patients still need to take medication, healthy living will reduce the risk of further complications as they grow older. Unfortunately, many diabetics persist with unhealthy behaviors, leading to out-of-range episodes which can impact their wellbeing and increase the risks of acute and long-term complications. This is often linked to:
- Lack of insight or personalized feedback on their lifestyle choices and environment.
- Low awareness of acceptable alternatives.
- Limited clarity on the benefits of early changes in small and achievable steps versus the costs of delay or denial.
Primary care clinics admit that they lack sufficient time during visits to guide their patients on adopting and maintaining healthy habits, acknowledging that more coaching could help in avoiding or compounding long-term risks.
Diameter: a virtual diabetes coach available on the Ancora platform
Enabling patients to better self-manage, and for healthcare practitioners to intervene in a timely manner in between visits, can help to manage diabetes care more efficiently while also improving patient experience and outcomes.
Evidence-based digital therapeutics for virtual care can offer a significant boost here. A good example is Diameter, an award-winning pathway developed by researchers at the University of Twente and ZGT hospital. Available exclusively on the Ancora platform, Diameter helps T2D patients to improve their lifestyle habits and glycemic control.
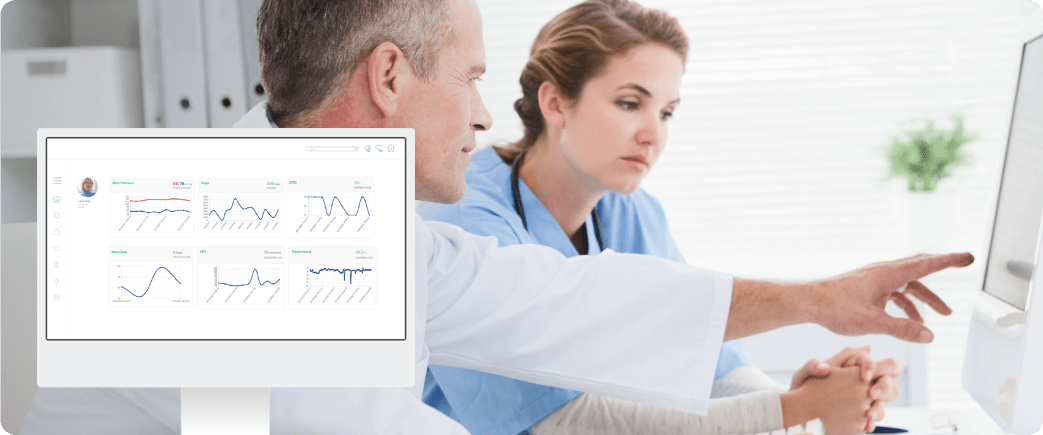
Patients on Diameter can use an app to
- Track their nutrition in a digital food diary, and physical activity via connected wearables (or self-reported).
- Record blood glucose values – self-reported or via sensors, including continuous glucose monitoring devices.
- Receive lifestyle and goal-setting advice and feedback through tailored recommendations.
Diameter’s digital coaching is based on the scientific application of empirical behavior change models. Patient data and responses from the app are relayed back to the hospital or clinic, where the care team can then reach out if they see a patient’s health data fluctuate beyond preset thresholds.
Diameter has already received two grants from Diabetes Fonds. Diabetes Fonds is now investing in a blended care platform, in which Diameter will play a key role. The platform will deliver personalized, proactive diabetes monitoring and management in a way that is easily accessible for patients and their healthcare practitioners.
Encouraging results from early users

“Thanks to the Diameter app, the amount of insulin I use to balance my sugar levels went down by 20 %”
– Ron la Faille –
The University of Twente and ZGT hospital piloted Diameter in 2021 with type 2 diabetes patients treated at the outpatient clinic of ZGT hospital. The patients used the Diameter app for 10 weeks – with encouraging results.
- Participants were extremely positive about Diameter’s self-monitoring functionalities as it provided new insights into how their glucose levels responded to adjustments they made to their lifestyle.
- Patients made frequent use of the app’s glucose monitoring functions over the 10 weeks, along with the coaching elements.
- Around 85% of the coaching exercises were completed whenever participants understood the purpose of the exercise. (A key lesson learnt was that the purpose behind each exercise must be made clear).
Quadruple aim impact
Diameter’s mix of technology and human supervision, i.e., the blended care approach – has the potential to improve population health outcomes, staff and patient experience while reducing the cost of care, explains Prof. Goos Laverman, Professor at the University of Twente, who is also Internist at ZGT hospital and one of the prime movers behind Diameter.
“Conventional treatment of diabetes is often reactive. Patients go for a scheduled check-up every few months, where their blood sugar levels are measured, and medication adjusted where needed; they have limited face time with their caregiver, may or may not comply with standard lifestyle advice. With Diameter, care becomes more proactive and personal because both patient and caregiver can track the impact that improved awareness and adherence to recommended lifestyle behaviors and goals are having on the condition, and the care team can therefore spend more time on those who need the most support. We may be able to reduce avoidable in-person visits since the data is already accessible, and interaction, if needed, is possible remotely through the platform and app – thus improving patient confidence and convenience, and reducing costs where applicable.”
Next steps
Although there is vocal support from public health authorities and stakeholders for digital transformation to reduce pressure on the healthcare system, the implications of virtualizing care pathways in terms of clinical workflows, deployment modalities, approval processes and payment models are still vague.
We at Ancora Health will work closely with the University of Twente and ZGT hospital to offer and support Diameter via the Ancora platform, starting with a pilot covering 200 patients at ZGT hospital. Diameter is also being tested in an ongoing clinical trial to evaluate its effectiveness as a blended care intervention in secondary care for patients with more complicated conditions. Separately, it also plays a key role in the PerfectFIT Platform for personalized behavioral change that is being set up and tested with support from the recent Diabetes Fonds grant.
After the pilot, our initial focus is to scale up the use and impact through wider hospital and primary care adoption in the Netherlands. A parallel step is to engage with insurers on evaluation criteria, and possibly contribute to their evolving approach around reimbursement of digital therapeutics, in this case for diabetes care.
“This is an exciting prospect for primary and secondary care as well as patients in the region, and potentially the entire Dutch healthcare system”, concludes Prof. G. Laverman. “Together with Ancora, we are committed to developing and scaling Diameter further to help improve outcomes for pressing population health challenges in a cost-effective manner, starting with type 2 diabetes.”
SUBSCRIBE
Subscribe to our mailing list to be among the first to know about our latest blogs.
Learn how Ancora handles your personal data in our privacy policy